Bio-Med 281
Cardiac Pathophysiology
Final Examination
September 25, 2000
ª ªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªª
I cannot teach anybody anything, I can only make them
think. -- Socrates
Murphy's Law of Copiers: The legibility of a copy is inversely
proportional to its importance.
Murphys Rule of Accuracy: When working toward the solution
of a problem, it always helps if you know the answer.
ª ªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªªª
The roots of education are bitter, but the fruit is sweet.
-- Aristotle
It aint over till its over. Yogi Berra
ª ªªª
Questions 1 5: A thirty-five year old male Egyptian
immigrant presents to the medical clinic for a pre-employment physical.
He states that he had no prior illnesses but has been having some dyspnea
on climbing stairs recently. On physical examination, his main finding
is that of a loud first heart sound, a high-pitched sound immediately after
S2, and a low-pitched diastolic murmur during diastole.
-
This patient is likely to have all of the following anatomical
or physiological findings, except:
-
a normal left ventricle
-
a dilated left atrium
-
thinned and elongated chordae tendinae
-
doming of the mitral valve leaflets
-
mildly elevated pulmonary artery pressures
2. The most likely etiology (cause) of this patients
abnormality is:
-
prior acute rheumatic fever
-
longstanding hypertension
-
acute "silent" myocardial infarction
-
congenital bicuspid aortic valve
-
bacterial endocarditis
3. The predominant physiological abnormality in
this patient is:
-
impaired emptying of the left ventricle
-
impaired filling of the left ventricle
-
volume overload of the left ventricle
-
pressure overload of the left ventricle
-
diastolic left ventricular dysfunction
Several months after this patient has started his job as
an accountant, he develops dyspnea while working on tax returns on April
14th. He presents to the employee health department where his
heart rate is noted to be rapid. He is sent to your office where an EKG
rhythm strip reveals the following rhythm:
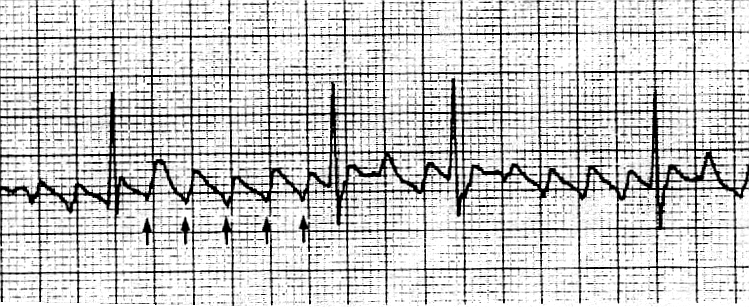
4. Identify the abnormal rhythm:
-
sinus tachycardia
-
atrial fibrillation
-
atrial flutter
-
ventricular fibrillation
-
ventricular tachycardia
5. The pathophysiological mechanism of this arrhythmia
is most likely:
-
increased automaticity in the atrium
-
increased automaticity in the A-V node
-
increased conduction through the A-V node
-
re-entry within the A-V node
-
re-entry within the atrium
Questions 6 7: A 75 year-old female has been under
treatment for arthritis with four weeks of non-steroidal anti-inflammatory
drugs. She now notes two days of increasing chest pressure with exertion
and black, tarry stools. On examination she appears pale and her vital
signs are: Pulse 110/min; BP: 90/60; Resp: 16; Temp: 98.6 F.
6. Pathophysiologic mechanisms for her accelerated
angina pectoris might include all of the following, except:
-
Increased myocardial oxygen demand due to sinus tachycardia
-
Increased left ventricular wall tension due to increased
preload
-
Increased myocardial contractility due to increased sympathetic
tone
-
Decreased diastolic coronary perfusion pressure due to hypotension
-
Decreased oxygen carrying capacity due to anemia
7. During episodes of chest pressure, all of the
following pathophysiologic mechanisms may be taking place, except:
-
increased local adenosine levels, causing local vasodilation
(to increase coronary blood flow)
-
increased local EDRF or nitric oxide levels, causing local
vasodilation (to increase coronary blood flow)
-
increased catecholamine production, causing increase in heart
rate and contractility (increasing myocardial oxygen demand)
-
increased external compression of the coronary vessels, causing
increased coronary vascular resistance
-
increased local cyclic-AMP levels, causing local vasoconstriction
(decreasing coronary blood flow)
Questions 8 13: A 4 year old boy is seen in the
office with parental complaints of inability to play with other children
for any length of time before tiring out. On exam his cheeks appear ruddy
with deep red lips. There is a loud, harsh systolic ejection murmur. The
patient has mild clubbing of the fingers and the EKG demonstrates right
ventricular hypertrophy.
8. The most likely diagnosis is:
-
ASD
-
VSD
-
transposition of the great arteries
-
tetralogy of Fallot
-
coarctation of the aorta
9 - 13: TRUE or FALSE: A chest X-ray examination of
this boy would likely show which of the following (more than one may be
correct):
-
pulmonary oligemia
-
cardiomegaly
-
lobar infiltrates
-
boot shaped heart
-
pulmonary edema
Questions 14 - 18: Match each
question with the single best answer (A - E).
|
14.
Decreased diastolic aortic pressure;
increased left ventricular end-diastolic pressure;
volume overload of the left ventricle;
bounding peripheral pulses
|
A
Constrictive Pericarditis
|
|
15.
Impaired diastolic filling of ventricles;
jugular venous pressure with rapid "y descent";
left ventricular diastolic pressure tracing with "dip
and plateau" configuration
|
B
Restrictive Cardiomyopathy
|
|
16.
Impaired diastolic filling of ventricles;
cyclical decrease in systolic blood pressure during inspiration;
elevated jugular venous pressure without Kussmauls sign
|
C
Aortic Regurgitation
|
|
17.
Impaired diastolic filling of the left ventricle; normal left ventricular
end-diastolic pressure;
increased pulmonary venous pressure with occasional "reactive" pulmonary
hypertension
|
D
Cardiac Tamponade
|
|
18.
Impaired diastolic filling of the ventricles; fibrosis,
scarring, or infiltration of the myocardium; normal pericardial tissue
|
E
Mitral Stenosis
|
19. The action potential of a pacemaker cell differs from that
of a cardiac myocyte in all of the following ways except:
A. phase 0 is due to slow Ca++ influx
B. maximum negative voltage is less negative (-60 mV)
C. the resting membrane potential is determined by voltage sensitive
ion channels
D. spontaneous depolarization occurs during phase 4
20. A 28 year-old woman presents with shortness of breath. Physical
examination reveals a grade II/VI diastolic murmur heard at the apex with
pre-systolic accentuation. Her EKG reveals a biphasic P wave in lead V1.
The terminal negative deflection of the P wave is 1mm wide by 1mm deep.
The diagnosis based on her P wave morphology is:
A. right atrial enlargement
B. left atrial enlargement
C. atrial flutter
D. left ventricular hypertrophy
21. Re-entry is the principle mechanism of arrhythmogenesis for
all of the following arrhythmias, except:
A. supraventricular tachycardia
B. atrial flutter
C. ventricular tachycardia
D. atrial fibrillation
E. torsades de pointes
22. The following are all true about a re-entrant circuit except:
A. it is a self-sustaining electrical circuit
B. requires unidirectional block in one limb of the circuit
C. requires rapid conduction through one limb of the circuit
D. can occur in the AV node
E. can occur in the left ventricle
23. A 58 year-old man with an ischemic cardiomyopathy presents
to the emergency room complaining of palpitations and dizziness. His heart
rate is 160 beats/min. On EKG, the QRS complexes are regular, wide and
bizarre. The P waves are visible but do not appear to have any relationship
to the QRS complexes. This patients rhythm is most likely:
A. ventricular fibrillation
B. ventricular tachycardia
C. atrial fibrillation
D. sinus tachycardia
24. Left ventricular compliance is reduced in all of the following
conditions, except:
-
Mitral stenosis
-
Aortic stenosis
-
Acute myocardial infarction
-
Restrictive cardiomyopathy
-
Dilated cardiomyopathy
Questions 25 31: A 55 year old male presents to the emergency
room with 2 hours of severe substernal chest pressure radiating to his
left arm, associated with dyspnea and diaphoresis. On EKG, he is noted
to have ST segment elevations in the precordial leads V1 to
V5.
25. Pathophysiologic mechanisms for this patients syndrome are likely
to include all of the following, except:
-
coronary embolism from the left atrium or left ventricle
-
intracoronary plaque rupture or fissuring
-
platelet aggregation on the plaque
-
intracoronary thrombus formation
-
local coronary vasospasm
57. Complications
of the patients syndrome over the next week might include any of the following,
except:
-
rupture of the free wall of the left ventricle, resulting in cardiac tamponade
-
ventricular tachycardia, leading to hypotension or ventricular fibrillation
-
congestive heart failure, due to decreased compliance and decreased cardiac
output of the left ventricle
-
rupture of the postero-medial papillary muscle of the left ventricle, resulting
in acute mitral regurgitation
-
rupture of the intra-ventricular septum, resulting in an acute ventricular
septal defect
This patients Frank Starling curve is represented below as the lower
of the two curves.
Please answer the next TRUE or FALSE questions based on this diagram
(A = TRUE ; B = FALSE).

26. This patients prognosis is better if he is on point A rather than
point B on the curve.
27. This patient can be moved from point B to point C by administering
fluids.
28. This patient can be moved from point A to point B by administering
a positive inotrope.
29. Patients falling into Quadrant IV have a mortality rate of less
than 30 percent.
30. Patients falling into Quadrant III usually have clear lungs and
low blood pressure.
Questions 31 33:
 Please match each of the
three labeled diagrams with their corresponding legends, by filling in
A, B, or C.
Please match each of the
three labeled diagrams with their corresponding legends, by filling in
A, B, or C.
31. These pressure-volume loops show the effect of increasing afterload
on stroke volume.
32. These pressure-volume loops show the effect of increasing preload
on stroke volume.
33. These pressure volume loops show the effect of adding an inotropic
agent on stroke volume.
Questions 34 - 35: A 70 year-old woman with a known heart murmur
and a history of atrial fibrillation has had progressive angina and dyspnea
on exertion. On physical exam she has a harsh crescendo/decrescendo murmur
at the left sternal border radiating to the right upper sternal border.
She is referred for a cardiac catheterization, and her hemodynamics are
noted below.

34. Appropriate therapy would include all
of the following except:
a. b - blockers
b. Ca 2+ -channel blockers
c. Disopyramide
d. Aortic valve replacement
e. Alcohol septal ablation
35. This patients heart murmur would be expected to do all of
the following, except:
-
increase with standing up from a squatting position
-
decrease with elevation of the legs while in a supine position
-
decrease with the Valsalva maneuver
-
increase after a premature ventricular contraction
-
decrease during pregnancy (if she were younger)
36. All of the following are features of pericardial tamponade except:
a. electrical alternans on EKG
b. pulsus paradoxus
c. pulsus alternans
d. equalized diastolic pressures
e. blunted "y" descent
37. A 55 year-old man presented with 2 weeks of increased shortness of
breath, chest pain, lower extremity edema and abdominal bloating. On exam
his BP was 80/60, his heart rate was 110 beats/min, and his jugular veins
were elevated to the angle of his jaw. His respiratory rate was 36/minute.
When palpating his pulse, it seemed to disappear with each inspiration.
His CXR showed a markedly enlarged cardiac silhouette, but clear lung fields.
Initial therapy should have included:
-
Furosemide 40mg IV
-
Sublingual Nitroglycerin
-
Metoprolol 5 mg IV
-
Normal saline 250 ml IV bolus
-
Dobutamine IV
38. True statements regarding the pathological time course in
acute myocardial infarction include all the following, except:
-
Yellow softening from resorption of dead tissue by macrophages generally
occurs within 36 hours of the infarction
-
Fibrosis and scarring generally occurs by two months after infarction
-
Irreversible cellular injury usually occurs within 20-30 minutes of the
onset of the infarction
-
ATP levels fall and regional systolic function drops within one to two
minutes of the onset of the infarction
-
Coagulation necrosis generally occurs within 24 hours of the onset of infarction
Imaging questions 39 43: Match each method appropriately.
|
39.
Imaging technique most effective in determining precise anatomical coronary
artery information
|
A
Resting thallium nuclear image
|
|
40.
Imaging technique most useful in visualizing valvular and sub-valvular
structures
|
B
Exercise and resting
thallium nuclear imaging
|
|
41.
Imaging technique most useful in determining severity of valve stenoses
non-invasively
|
C
2-D echocardiography
|
|
42.
Imaging technique most useful in determining significance of coronary
stenoses non-invasively
|
D
Doppler examination
during 2-D
echocardiography
|
|
43.
Imaging technique most useful in determining myocardial viability non-invasively
|
E
Cardiac catheterization
(coronary angiography)
|
44. Right ventricular infarction is associated with all of the following
findings, except:
-
Clear lung fields with jugular venous distension
-
A left ventricular S3 gallop
-
Hypotension responding to fluid administration
-
Inferior wall myocardial infarction
-
Elevated right atrial pressure, almost equal to PCW (wedge) pressure
45. Acute ventricular septal rupture occurring several days after myocardial
infarction is associated with all of the following, except:
-
Yellow softening in the area of the intraventricular septum
-
Oxygen saturation "step-up" from the right atrium to the pulmonary artery
-
A loud systolic and diastolic "to-and-fro" murmur at the left sternal border
-
A systolic "thrill" which is palpable at the left sternal border
-
Signs and symptoms of congestive heart failure
Questions 46 50: Match each term with the appropriate definition
|
46. {Pressure x Radius} / {2 x wall
thickness}measured during systole
|
A
Preload
|
|
47. {Pressure x Radius} / {2 x wall
thickness}measured during diastole
|
B
Afterload
|
|
48. {Pressure x Radius} / {2 x wall
thickness}measured at any point in time
|
C
Wall tension
|
|
49. Change in pressure / Change in
volume
|
D
Compliance
|
|
50. Change in volume / Change in pressure
|
E
Stiffness
|
51. The Fick Method of determining cardiac output predicts all of the
following, except:
-
An increase in mixed venous oxygen saturation suggests an increase in cardiac
output
-
A decrease in oxygen consumption suggests an increase in cardiac output
-
The cardiac output can be estimated using three parameters: the oxygen
consumption, the arterial oxygen saturation and the mixed venous oxygen
saturation
-
The calculation of the cardiac output using the Fick method is independent
of the ability of the lungs to oxygenate the blood
52. Acute mitral regurgitation differs from chronic mitral regurgitation
in all of the following ways, except:
-
Acute mitral regurgitation (MR) results in large V-waves on the pulmonary
capillary wedge tracing, while chronic mitral regurgitation does not
-
Acute MR is more likely to present as acute pulmonary edema than chronic
MR
-
Acute MR often occurs due to an acute inferior MI, while chronic MR is
usually due to other causes
-
Acute MR causes a systolic ejection murmur, while chronic MR causes a holosystolic
"plateau" murmur
-
Acute MR is effectively treated with afterload reduction, while chronic
MR is not
Questions 53 - 56: Match the following signs/symptoms with their etiology
|
53.
Bisfiriens pulse
|
A
CardiacTamponade
|
|
54.
Pulsus Alternans
|
B
Aortic Stenosis
|
|
55.
Pulsus paradoxus
|
C
Hypertrophic Cardiomyopathy
|
|
56.
Pulsus tardus et parvus
|
D
Dilated Cardiomyopathy
|
57. See above (25 b)
Answers
to 2000 EXAM



 Please match each of the
three labeled diagrams with their corresponding legends, by filling in
A, B, or C.
Please match each of the
three labeled diagrams with their corresponding legends, by filling in
A, B, or C.
