
|
August 28, 2006 |
Death of a Parasite: Stripped, Surrounded, Consumed
For the first time, a group of researchers has shown that a parasite can be eliminated through autophagy, a recycling process that normally occurs inside cells. The team, led by George Yap of Brown University, shows that the immune system destroys and disposes of the parasite Toxoplasma gondii by stripping it naked then gobbling it up. | |||
|
Brown University Home |
PROVIDENCE, R.I. — As much as 65 percent of the world’s population may be infected by Toxoplasma gondii, a crafty one-celled parasite often carried by cats. The parasite, however, rarely causes illness in humans because the immune system keeps it in check – and because the parasite can, in a clever way, avoid detection. When Toxoplasma gondii is found out, how does the immune system kill it? Through a grisly process, according to research led by Brown University immunobiologist George Yap. The intracellular parasite is stripped, surrounded and devoured using autophagy, a strange self-eating process cells use to remove and reuse old or damaged parts. 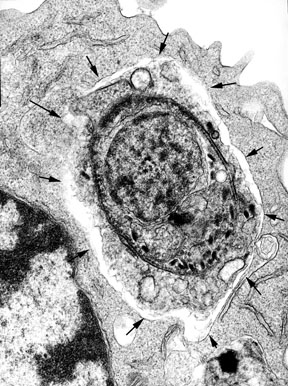 Exposed and defenseless The research by Yap and colleagues, which appears in the Journal of Experimental Medicine, is the first to detail, step-by-step, how Toxoplasma gondii and other members of its parasite class are killed off by the immune system. It’s also the first to show that parasites can be disposed of through autophagy, a cellular recycling process of increasing interest to scientists. Autophagy allows for healthy cell growth and development and appears to suppress, or in some cases aid, cancerous tumors. But new research is showing that autophagy can also kill invading pathogens. “There is the saying that ‘nature is thrifty,’ and we’re seeing that at work here,” Yap said. “We found that the body uses an old trick – autophagy – for this new purpose. It’s just become clear in the last two years that autophagy can kill viruses and bacteria, such as the kind that cause tuberculosis. Now we know that the process can destroy parasites too.” Autophagy’s newfound ability to consume disease-inducing invaders has even spawned a new term – xenophagy, whose prefix means foreign. Toxoplasma gondii is an apicomplexan, a class of parasites that also includes the malaria parasite as well as Cryptosporidium, which causes a common form of intestinal diarrhea. These parasites are stealthy – which makes them successful. When they enter cells, Yap explained, the parasites build a safe house of sorts. The membrane sac, or vacuole, lacks the receptors that would allow lysosomes, the cell’s gobbling garbage collectors, to attach themselves and start feasting. So how does the immune system destroy such a cunning opponent? Researchers used macrophages, white blood cells triggered by the immune system, to find out. They activated the cells and inserted the parasites. They found that interferons, proteins produced by cells of the immune system, switch on a gene called IGTP. While the precise role of the gene is a mystery, the Yap team found that activation of IGTP is critical, prompting the macrophage to form finger-like appendages that literally feel out the parasite inside its safe house. These “fingers” then pull at the membrane, or frame, of the house until it disintegrates. The parasite is completely exposed. Then, through an unknown mechanism, the macrophage peels off the parasite’s membrane, akin to skinning it. Now autophagy kicks in. The naked bug, spilling its innards, is enveloped in two membrane sacs. This, however, is no safe house. The outer sac contains the receptors that lysosomes can attach to. Once the lysosomes arrive, they consume the parasite’s remains. “It’s a surprisingly aggressive process,” Yap said, “and it shines a light on this black box. Now that we better understand this destructive process, the question is: Can you induce it with a drug? If so, that drug could provide protection from all sorts harmful pathogens.” Brown graduate students Yun Ling and Michael Shaw, both in the Department of Molecular Microbiology and Immunology, worked on the experiments along with Carol Ayala, a Rhode Island Hospital microscopist. Isabelle Coppens at the Johns Hopkins School of Public Health, Gregory Taylor at Duke University and David Ferguson of Oxford University also were members of the research team. The National Institute of Allergy and Infectious Diseases funded the work. ###### | |||