BIO-MED 350
COMBINED CARDIAC PATHOPHYSIOLOGY,
PHARMACOLOGY & PATHOLOGY EXAM
2006
Questions 1 -
9:
A 54 year old male presents to the
hospital with progressive symptoms of shortness of breath. Physical examination reveals a systolic
heart murmur and lung findings consistent with congestive heart failure. An
echocardiogram is performed and reveals a significant cardiac structural
abnormality.
For further diagnosis, a cardiac
catheterization is performed, and the following tracing is obtained while
pulling back the catheter from the left ventricular apex to the
aorta:
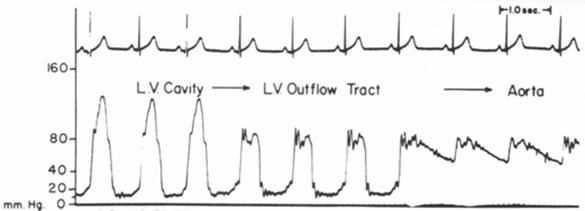
1. This patient’s cardiac structural
abnormality most likely represents:
A) mitral
stenosis
B) aortic
stenosis
C) hypertrophic cardiomyopathy with
LV outflow
obstruction
D) pulmonic
stenosis
E) coarctation of the
aorta
Questions 2 -
7:
Please indicate (true or false),
whether each of the following is associated with this patient’s
condition:
2. Impaired systolic LV function
3. Impaired diastolic LV function
4. Increased risk of sudden cardiac
death
5. Mitral regurgitation
6. Delayed and diminished carotid
upstrokes
7. Reduction of heart murmur intensity with standing
up
Annotated answers
to Questions 1 - 9:
This case represents a
classic case of hypertrophic cardiomyopathy with outflow tract obstruction, in
which a gradient is seen between the
LV apex and the LVoutflow tract. This has been identified during the
catheter pullback as a drop in systolic pressure within the
LV cavity.
This condition is associated with
normal to hypernormal systolic function with impaired
LV relaxation, or diastolic
dysfunction. It is also associated with an increased risk of sudden cardiac
death. There is often associated mitral regurgitation, due to systolic anterior
motion of the mitral valve, resulting in functional MR. Classic physical exam findings include a
bisferiens pulse and a systolic ejection murmur which
increases with standing and with Valsalva maneuver.
Delayed and diminished carotid
pulses (pulsus “parvus et
tardus”) are associated with aortic
stenosis.
ANSWERS: 1.
C 2. B 3. A 4. A 5.
A 6. B 7. B
The following sets of tracings are
obtained before and after an intervention:
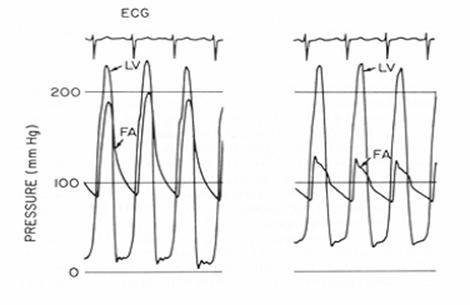
BEFORE AFTER
8. The most likely
intervention to cause this change in pressures was:
A) Valsalva
maneuver
B) Squatting
C) Passive leg
raising
D) Volume infusion with normal
saline
This same patient develops palpitations
and lightheadedness. An EKG reveals rapid atrial fibrillation with a ventricular
response rate of 130 beats per minute.
9. All of the following medications may
help slow his heart rate, except:
A)
Amlodipine
B)
Diltiazem
C)
Verapamil
D)
Digoxin
E) A
beta-blocker
Answers to Questions 9 & 10: 9.
A 10. A
*************************************************************************
10. The best drug to use for rapidly
controlling the ventricular response in a patient with new onset atrial
fibrillation is:
A) digoxin
B) amiodarone
C) verapamil
D) adenosine
E) flecainide
Answer: C
11. Which of the following statements best describes
the normal conduction of electrical impulses through the AV
node?
A) Transmembrane calcium currents are responsible for
activation of AV nodal cells, resulting in relatively slow conduction, in
comparison to working ventricular myocytes.
B) Transmembrane sodium currents are responsible for
activation of AV nodal cells, resulting in relatively slow conduction, in
comparison to working ventricular myocytes.
C) Parasympathetic stimulation has little effect during
the resting state on the behavior of AV nodal cells
D) Sympathetic stimulation has little effect during the
resting state on the behavior of AV nodal cells
Answer: A
12. The mechanism responsible for the majority of
pathologic clinical cardiac arrhythmias is:
A) Intramyocardial reentry due to functionally-based
circuits.
B) Intramyocardial reentry due to anatomically-based
circuits.
C) Triggered activity due to delayed
afterdepolarizations.
D) Triggered activity due to early afterdepolarizations.
E) Abnormal
automaticity
Answer: A
13. The major antiarrhythmic actions of digitalis
are due to:
A) Sympathetic
blockade
B) Inhibition of the Na/K ATPase
pump
C) Parasympathomimetic
actions
D) Improvement in ventricular function
resulting from its positive inotropic effects.
Answer: C
14. Which of the following agents
should never be used to treat atrial fibrillation in a 50 year old man who
experienced myocardial infarction 5 years previously:
A) Digitalis
B) Verapamil
C) Dofetilide
D) Flecainide
Answer: D
15. Development of a prolonged QT interval and
torsade de pointes is unlikely to occur with which of the following
antiarrhythmic agents?
A) Procainamide
B) Amiodarone
C) Quinidine
D) Verapamil
Answer:
D
**************************************************************
Questions 16 -
22:
A 75 year-old Middle
Eastern female presents to the hospital with progressive fatigue, abdominal
swelling and ankle edema. She has gained over 25 pounds over the last
month, and has been sleeping in a recliner chair.
The patient relates a remote
history of tuberculosis, which has been treated and “eradicated”.
On examination, her jugular veins
are distended, her lung fields are clear, and she has evidence of ascites and
peripheral edema.
Right heart catheterization is
performed and the following tracings are obtained (RA = right atrium; RV = right
ventricle; LV = left
ventricle):
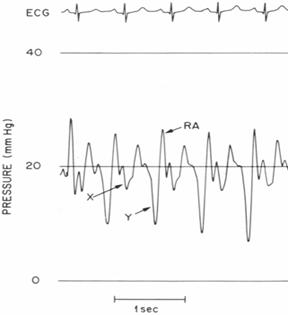
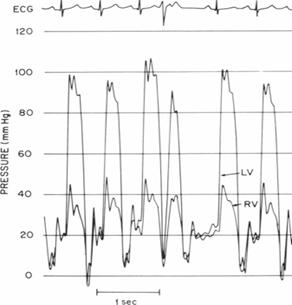
The patient is likely to manifest each
of the following features:
( A/True or B/False ):
16. Kussmaul’s
sign
17. Pulsus paradoxus
18. Equalization of diastolic
pressures
19. Auscultatory finding of
a pericardial “Knock”
20. Reduced forward cardiac
output
21. Calcification of the heart border on Chest
X-ray
22. Reduced left ventricular systolic
function
Q. 16 – 22: This is a classic case of a patient with
constrictive physiology – rapid y descent on the RA tracing, and equalization of
LV and RV diastolic pressures, with
a “square root sign” during diastolic filling of the ventricles.
Pericardial constriction is
associated with all of the following:
Kussmaul’s sign
A pericardial knock
Equalization of diastolic pressures
Rapid y descent
Reduced cardiac output due to decreased
LV filling
Calcification of the heart border on chest X-ray
It is usually not associated
with pulsus paradoxus, and
isolated LV systolic function
remains normal – the LV is just
underfilled.
ANSWERS
16 – A
17 – B
18 – A
19 – A
20 – A
21 – A
22 – B
*********************************************************************************
Questions 23 - 31:
A forty five year old male with
history of hypertension, high cholesterol and cigarette smoking presents to the
emergency room with severe mid-sternal chest “heaviness”, radiating to his neck
and arms, of one hour’s duration.
An electrocardiogram reveals
ST-segment elevation in the inferior leads.
On examination, the patient’s
pulse is slow, 50 beats per minute, and the blood pressure is mildly reduced, at
90/60 mm Hg.
23. Causes of this patient’s
bradycardia (slow heart rate) might include all of the following,
except:
A) a re-entry circuit within the left
ventricle
B) sinus node
ischemia
C) A-V node ischemia, causing Mobitz I
(Wenckebach) 2nd degree block
D) Increased vagal (parasympathetic)
tone
E) A-V node ischemia, causing 3rd degree
AV block with a junctional escape rhythm
24. The most
likely major contributing cause to this patient’s low blood pressure at the
present time is:
A) Acute mitral regurgitation from
papillary muscle rupture
B) Acute right ventricular infarction, causing decreased
LV preload
C) Significant left ventricular
infarction, causing markedly reduced LV stroke
volume
D) Acute ventricular septal
rupture
E) Pericardial tamponade from
LV free-wall
rupture
25. All of the following statements
about this patient’s acute myocardial infarction are true,
except:
A) the “ischemic cascade” starting at the
onset of his myocardial infarction includes diastolic dysfunction, systolic
dysfunction, EKG changes and chest pain
B) the myocardial infarction proceeds in a “wavefront” manner, proceeding
from epicardium to endocardium
C) systolic dysfunction caused by the
infarction may lead to further ischemia by decreasing coronary perfusion
pressure
D) diastolic dysfunction caused by the
infarction may lead to increased wall tension and decreased oxygen delivery to
the myocardium
E) sympathetic stimulation due to the pain
of the infarction may increase myocardial oxygen demand
(MVO2)
Several days after the patient’s
initial myocardial infarction, the patient develops worsening shortness of
breath and is noted to have a new, harsh systolic murmur. Right heart catheterization reveals the
following findings:
|
|
Oxygen
Saturation |
Pressure (mm
Hg) |
|
Right
Atrium |
70% |
8 |
|
Right
Ventricle |
72% |
40/8 |
|
Pulmonary
Artery |
71% |
40/22 |
|
Pulmonary Capillary
Wedge |
|
25 mean
V-waves to
50 |
26. This patient’s echocardiogram might
be expected to show:
A) Acute mitral regurgitation
B) Acute ventricular septal
defect
C) Acute right ventricular
infarction
D) Cardiac
tamponade
E) Apical LV aneurysm
formation
27. Treatment of the patient at this
time might include all of the following, except:
A) administration of thrombolytic therapy
B) emergency cardiac
catheterization
C) placement of an intra-aortic balloon
pump
D) surgical consultation for possible
open-heart surgery
E) vasodilatory drugs to augment forward
cardiac output
28. Intra aortic balloon pump placement
may do all of the following, except:
A) Reduce LV afterload
B) Reduce LV preload
C) Increase coronary blood
flow
D) Reduce myocardial oxygen
demand
E) Increase cardiac
output
Unfortunately, despite your team’s best
medical efforts, the above patient dies of congestive heart failure. The
following photograph shows a cross-section of the patient’s right coronary
artery. Please answer the questions below the
photo.
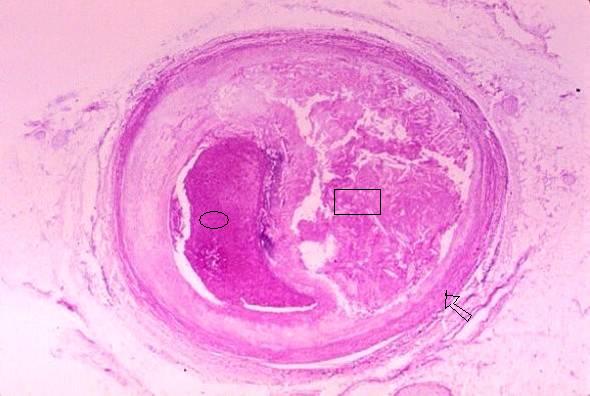
29. The object indicated by the oval
is:
A)
the central core of an atherosclerotic
plaque
B)
a thrombus occluding the lumen of the
artery
C)
a large
calcium deposit in a thickened intima
30. The rectangle is positioned in:
A)
a
thrombus occluding the lumen of the artery
B)
a
large calcium deposit
C)
the central core of an atherosclerotic
plaque
31. The arrow points
to:
A) the media
B) the intima, which in that location is
uninvolved
C) the adventitia
Questions 32 - 37:
A patient presents to the hospital with an acute
anterior myocardial infarction associated with congestive heart failure. A right
heart catheterization is performed in the CCU.
This patient’s Frank Starling curve is represented
below as the lower of the two curves below.
Please answer the next TRUE or
FALSE questions based on this diagram (A = TRUE; B = FALSE).
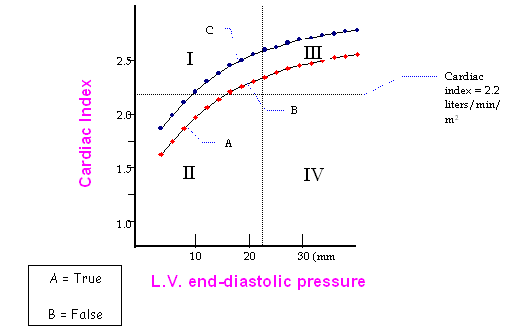
32. This patient’s prognosis is
worse if he is on point A rather than point B on the curve.
33. This patient can be moved
from point B to point C by administering fluids.
34. This patient can be moved
from point A to point B by administering fluids.
35. Patients falling into
Quadrant IV have a mortality rate of less than 30 percent.
36. Patients falling into
Quadrant III usually have pulmonary congestion and a normal blood
pressure.
37. Patients in Quadrant II have
the worst prognosis of all.
Answers: 32. A 33. B
34. A 35. B 36. A 37. B
Questions 38 - 40:
A 48-year-old Saudi Arabian female with a history of
rheumatic fever at age 20 presents to the office with progressive fatigue and
dyspnea on exertion. Physical examination reveals:
Heart rate: 90, regular; Blood
Pressure: 120/70; Respirations:
18
Neck: 8
cm JVD with prominent jugular V-waves; normal carotid
upstrokes
Chest: Fine rales at the
bases
Cor:
Prominent S1, increased pulmonic component of S2; high-pitched snap
shortly after S2; soft, II/VI systolic blowing murmur at the left sternal
border, increasing with inspiration; soft diastolic rumble with pre-systolic
accentuation
Extremities: trace edema; no
cyanosis
38. One would expect that this patient’s valvular
abnormalities would include:
A) Mitral stenosis and tricuspid
insufficiency
B) Aortic insufficiency and mitral
regurgitation
C) Aortic stenosis and mitral
regurgitation
D) Mitral stenosis and aortic
insufficiency
E) Hypertrophic cardiomyopathy with outflow tract
obstruction
39. On echocardiography, one would expect that this
patient’s left ventricle would demonstrate:
A) Concentric left ventricular
hypertrophy
B) Cavity dilation and global left ventricular
hypokinesis
C) Normal cavity size and normal left ventricular
function
D) Discrete sub-aortic septal
hypertrophy
E) Normal left ventricular size, with severe
global hypokinesis
40. Cardiac catheterization might demonstrate a
gradient between which two pressures:
A) Left ventricular and pulmonary capillary wedge
pressure during diastole
B) Ascending aortic pressure and
left ventricular pressure during systole
C) Right atrial and right ventricular pressure
during diastole
D)
Right ventricular and pulmonary artery
pressure during systole
Q. 38 – 40:
This is a somewhat difficult
question, in which a patient with a remote history of rheumatic fever develops
mitral stenosis, leading to right heart failure and secondary tricuspid
regurgitation.
The clues to these diagnoses
are:
Systolic blowing murmur
which accentuates with inspiration indicates tricuspid regurgitation. Also, the
prominent jugular V-waves indicate TR. The diastolic rumble with pre-systolic
accentuation is classic for mitral stenosis.
Despite the signs of
right heart failure, the left ventricular function in mitral stenosis is usually
normal. There is a gradient between the
LV and the PCW during
diastole.
PHARMACOLOGY QUESTIONS:
41. An 82 year-old woman presents to the Emergency
Room with a history of new-onset syncope. Upon arrival, she is awake and
oriented and has a small laceration on her forehead. Her blood pressure is
165/86 mmHg and her heart rate is 43 beats /minute. She is receiving unknown
medications for chest discomfort provoked by exertion and relieved by rest.
Which of the following combinations of drugs would most likely explain this
patient’s presentation?
A)
Diltiazem, nitroglycerin
spray
B)
Verapamil, Atenolol, Isosorbide dinitrate
C)
Nifedipine, Isosorbide
Mononitrate patch
D)
Amlodipine, sublingual
nitroglycerin
42. Indicate which of the choices below describes
the effects of a competitive antagonist on drug ED50 and
efficacy.
A)
A
decrease in ED50 with no change in efficacy
B)
A
decrease in ED50 and a decrease in efficacy
C)
No change
in ED50 and a decrease in efficacy
D)
An increase in ED50 and no change
in efficacy
E)
An
increase in ED50 and an increase in efficacy
43. An example of a ligand-gated
receptor:
A)
Muscarinic receptor
B)
b-1
receptor
C)
Nicotinic
receptor
D)
b-2
receptor
E)
a-1
receptor
44. Indicate which of the drugs below has the
greatest potency for producing ganglionic blockade:
A)
Trimethaphan
B)
Propranolol
C)
Atropine
D)
Pralidoxime (2-PAM)
E)
Acetylcholine
45. Indicate which of the agents below is used most
often to help diagnose myasthenia gravis:
A)
Atropine
B)
Trimethaphan
C)
Pancuronium
D)
Mecamylamine
E)
Edrophonium
46. All of the following statements regarding
neuromuscular blockers are correct EXCEPT:
A) Atracurium is a
competitive blocker
B) Succinycholine-induced blockade can be reversed by
acetylcholinesterase inhibitors
C) Anesthesia with halothane enhances competitive
blockade
D) Competitive blockers do not cross the blood-brain
barrier
E) Atracurium-induced
blockade can be reversed by acetylcholinesterase
inhibitors
True/False Questions:
47. When a partial agonist is
administered together with a full agonist, the response will be less than that
achieved compared to when the full agonist is given alone.
T
48. Following peripheral administration
of the two drugs, neostigmine has better access to the brain compared to
physostigmine.
F
49. For receptor binding of a ligand to
a receptor measured in the test tube, a linear plot of ligand bound on the
y-axis vs. a linear plot of ligand concentration on the x-axis produces a
sigmoid (S-shaped) curve.
F
50. Drug A has a lower ED50 compared to Drug B for a
specific response. Therefore
Drug A has a greater potency compared
to Drug B for this response.
T
51. All G-protein coupled receptors
produce their cellular responses by altering cyclic AMP levels in the cell.
F
Mr. Mucho Regurgitation has
recently had a successful mitral valve
replacement operation for severe
mitral regurgitation. His
echocardiogram 3 months after his open-heart
surgery showed a good
functioning prosthetic mitral valve, but an enlarged
left ventricle with
an ejection fraction of 35% and global hypokinesis. He
does not complain
of any symptoms of heart failure, and is walking daily
with a very good
functional status.
52. Which of the following drugs
would be expected to
have the SMALLEST or NO benefit on his long term
survival?
A. Carvedilol
B. Enalapril
C. Digoxin
D. Lisinopril
E. Sustained Release Metoprolol
53. Which of the following statements regarding the
cholinergic system is correct?
A. Acetylcholine is the transmitter released by
postganglionic sympathetic neurons
B. The most important mechanism
for removal of acetylcholine from the synaptic cleft is enzymatic
metabolism
C. Stimulation of the M2 muscarinic receptor in the heart leads to increased
myocardial contractility
D. Administration of methacholine is likely to produce bronchodilation in a patient with
asthma
E. Only two muscarinic receptor types (M1 and M2) are known to exist in
humans
54. A 70
year-old man has slowing of conduction in his atrioventricular (AV) node resulting in a significant
reduction in his ventricular rate and hypotension. Given this information, which of
the following medications would be most appropriate for this patient?
A) Acetylcholine
B) Pyridostigmine
C) Atropine
D) Ipatropium
E) Pilocarpine
55.
Parasympathomimetic drugs are categorized as either direct-acting or
indirect-acting. Which of the
following statements is correct?
A) Pilocarpine is an example of an indirect-acting
parasympathomimetic drug
B) A direct-acting parasympathomimetic drug works
by directly blocking the muscarinic receptor on the
target organ
C) An indirect-acting parasympathomimetic drug
works by decreasing the breakdown of acetylcholine
D) Donepezil (Aricept)
is an example of a direct-acting parasympathomimetic
drug
E) Both direct- and indirect-acting parasympathomimetic drugs are approved for the treatment of
gastrointestinal hypermotility
56. Which
of the following statements is correct regarding the autonomic nervous
system?
A) The sympathetic nervous system arises primarily from craniosacral outflow tracts
B) The division of the autonomic nervous system activated in response to
emotional and physical stress is called the parasympathetic nervous
system
C) The primary catecholamine released by chromaffin cells in the adrenal medulla is
epinephrine
D) Nicotine is the neurotransmitter released by preganglionic neurons
E) The neurotransmitter released by postganglionic parasympathetic neurons
is norepinephrine
A 24 year
old man arrives at the emergency room after taking an overdose of
amphetamines. His blood pressure is
180/100 and his heart rate is 120.
57. What is the mechanism of his
hemodynamic changes?
A) Direct effects of amphetamine on alpha-1 and beta-1 receptors.
B) Increased stimulation of presynaptic alpha-2
receptors.
C) Increased release
of norepinephrine into the synaptic cleft.
D) Inhibition of reuptake of norepinephrine from
the synaptic cleft.
A 70 year
old man is being started on terazosin for symptoms
related to his benign prostatic hyperplasia. He has no other medical diagnoses.
58. Which
of the following adverse effects should you warn him about?
A) Dizziness caused
by low blood pressure
B) Excessively slowed heart rate caused by direct effects on the SA
node
C) Constipation caused by relaxation of GI smooth muscle
D) Shortness of breath caused by bronchoconstriction
All
available beta-adrenergic antagonists block beta-1 receptors but their
administration may result in different therapeutic or adverse outcomes due to
additional properties.
59. Which of the following is
INCORRECT?
A) Due to its blockade of beta-2 receptors, propranolol should not be administered to patients with
asthma.
B) Intrinsic sympathomimetic activity (ISA) of
pindolol causes a relative increase in resting heart
rate during sleep.
C) Concurrent
blockade of alpha-2 receptors by carvedilol increases
the likelihood of hypotension with the drug.
D) While membrane-stabilizing activity is a characteristic of propranolol, it is not apparent at therapeutic
doses.
60. An 85
year old man with Alzheimer's Disease is given donepezil.
Which of the following should you anticipate as an adverse effect of the
drug?
A) Constipation
B) Urinary
incontinence
C) Dry eyes
D) Sinus tachycardia
61. Which
of the following statements is correct regarding the parasympathetic nervous
system?
A) Acetylcholine is synthesized in the postganglionic neuron and is released
passively into the synaptic cleft.
B) Activation of
presynaptic M1 receptors decreases release of
acetylcholine into the synaptic cleft.
C) Removal of acetylcholine from the synaptic cleft is primarily through
reuptake and the process is inhibited by cocaine.
D) Stimulation of M3 receptors in the heart result in decreased calcium
permeability and slowing of heart rate and AV nodal conduction.
62. A 6
year old child is seen in the emergency room and has signs of severe
organophosphate poisoning after ingesting an unknown quantity of pesticide. Which of the following statements is
correct?
A) Organophosphates
are classified as irreversible cholinesterase
inhibitors.
B) Atropine improves symptoms in patients with organophosphate poisoning by
increasing production of acetycholinesterase.
C) Respiratory muscle fatigue and paralysis are effectively treated with
high doses of atropine.
D) Due
to its toxicity profile, pralidoxime should be
withheld for the first 24 hours.
63. A 52 year-old male presents to your
office with complaints of exertional chest pressure, which occurs either with
physical activity or with emotional upset. You diagnose him with angina pectoris
and initiate treatment.
Therapy for angina may work by all of the following
mechanisms, except:
A) reducing preload, thereby decreasing wall stress,
decreasing MVO2
B) reducing heart rate, thereby reducing
MVO2
C) reducing blood pressure, thereby reducing wall
stress, decreasing MVO2
D) dilating coronary arterioles, thereby increasing
coronary blood flow
E) increasing contractility, thereby
increasing coronary blood flow
64. For which of the following anti-anginal agents
has a secondary prevention benefit been
demonstrated?
A) Isosorbide
dinitrate
B) Sublingual
nitroglycerin
C) Metoprolol
D) Amlodipine
E) Diltiazem
65. The mechanism of action of ranolazine
is:
A) Reduces blood pressure and therefore myocardial
oxygen consumption
B) Reduces both heart rate and blood pressure and
therefore reduced myocardial oxygen consumption
C) Increases coronary blood
flow
D) Is unknown but may involve glucose
metabolism
66. As part of the patient’s treatment,
anti-platelet therapy is also administered. Which of the following agents
interferes with the binding of ADP to its platelet
receptor?
A) Abciximab
B) Clopidogrel
C) Aspirin
D) Eptifibitide
Questions 67 - 71:
A 35 year old female presents to the hospital four
weeks after delivering her second child, with signs and symptoms of congestive
heart failure. Left ventricular ejection fraction is measured at 25% by bedside
echocardiography. Regarding her diagnosis of
cardiomyopathy:
67. Ischemic cardiomyopathy and non-ischemic
cardiomyopathy have all of the following features in common,
except:
A) Decreased left ventricular
compliance
B) Decreased left ventricular systolic
function
C) Compensatory left ventricular
dilation
D) Compensatory increase in circulating
catecholamines
E) Diffuse sub-epicardial left
ventricular necrosis
68. In patients such as this, one is likely to find
all of the following, except:
A) Pulsus alternans
B) Cardiomegaly
C) Increased
LV end-diastolic pressure
D) Coolness of the
extremities
E) Pulsus paradoxus
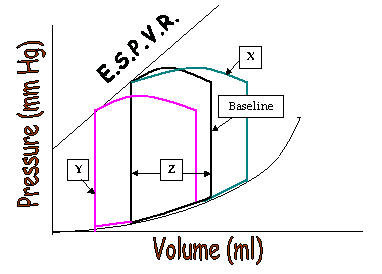
This patient is represented by the Pressure-Volume
loop shown above, labeled “Baseline”:
69. The pressure-volume
loop labeled "Y" might be generated by:
a. giving volume
b. giving an
ACE-inhibitor
c. giving a
diuretic
d. giving an inotropic
agent
70. The patient may have
gone from the loop labeled “X” to her current “baseline”
by:
A) Giving
volume
B) Giving an inotropic
drug
C) Giving
a diuretic
D) Giving an
ACE-inhibitor
E) Giving
hydralazine
The distance “Z” may be increased by doing all of
the following, except:
A) Increasing only
contractility
B) Increasing only
afterload
C) Increasing only preload
D) Giving an ACE-inhibitor
PATHOLOGY
QUESTIONS:
In the
photo below, the fetal heart has been rotated to the right.

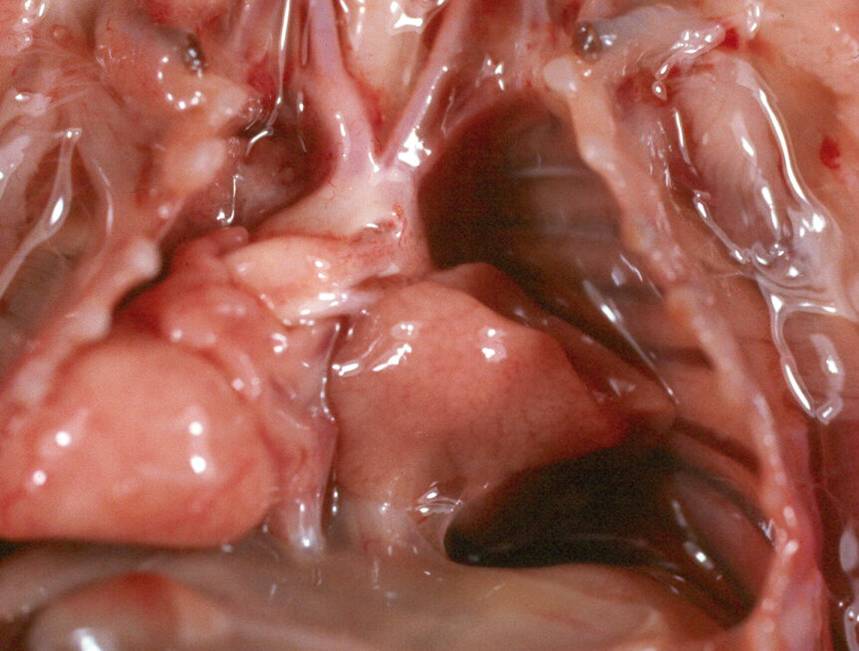
Answer
true (A) or false (B) for each of the following questions
about the structure marked with a white square.
(1 point each)
In a
normal fetus, it carries well-oxygenated blood, a large portion of which enters
the aortic arch and supplies blood flow to the brain. B
Postnatally, in the presence of certain cardiovascular
anomalies prostaglandin is given to maintain patency. A
In a
normal fetus, the amount of blood flow through this structure is only 25% as
great as flow through the pulmonary arteries.
B
Answer
true (A) or false (B) for the following statement: (1 point)
One of
the features which differentiates the left ventricle
from the right ventricle is a smooth upper septal surface with no attached chordae tendineae. A
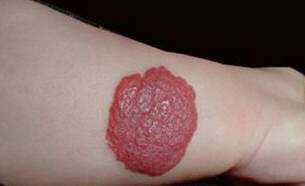
The
lesion illustrated above was on the extremity of an infant. Microscopically it
showed aggregates of thin-walled capillaries, closely packed and lined by
endothelium. No capsule was present.
Which of the following is a correct statement regarding this lesion?
(3 points)
A) Though this patient was an infant, this entity is most common in middle
age
B) This is the most common vascular tumor and can present as a
“strawberry type” in newborns
C) The lesion is always flat with no elevation
D) These lesions occur only in skin and mucous membranes
*************************************************************
Answer true (A) or false
(B) for each of the following
statements. (1 point
each)
Dilated
cardiomyopathy and myocarditis are entirely unrelated
entities.
B
Myocardial disarray is a microscopic feature of hypertrophic
cardiomyopathy. A
Among the
causes of dilated cardiomyopathy is chronic consumption of alcohol. A
Lymphocytic myocarditis is usually
secondary to drug hypersensitivity. B
Which of
the following vasculitides is not associated with antineutrophil cytoplasmic
antibodies (ANCA)?
(1 point)
A) Polyarteritis nodosa
B) Churg-Strauss syndrome
C) Wegener granulomatosis
D) Microscopic polyangiitis
Match the
region of the heart with the coronary vessel supplying oxygenated blood to that
region when the coronary circulation is right dominant. (1 point
each)
82. The
anteroseptal region B
83. The
posterior wall of the left ventricle
A
84. The
AV bundle and the posterior aspect of the upper septum A
85. The
lateral wall of the left ventricle C
A) Right coronary artery
B) Left anterior descending coronary artery
C) Left circumflex coronary artery
D) The coronary sinus
The least likely association with mitral
annular calcification is - (1 point)
A) Calcification of the aortic cusps
B) Calcification extending into the cardiac skeleton (central fibrous
body)
C) The presence of a parathyroid tumor causing hypercalcemia
D) Old age
A random Pathophysiology
Question:
Which of the following is not a
determinant of myocardial oxygen demand (MVO2)?
a) heart
rate
b) contractility
c) preload
d) hemoglobin
content
e) afterload
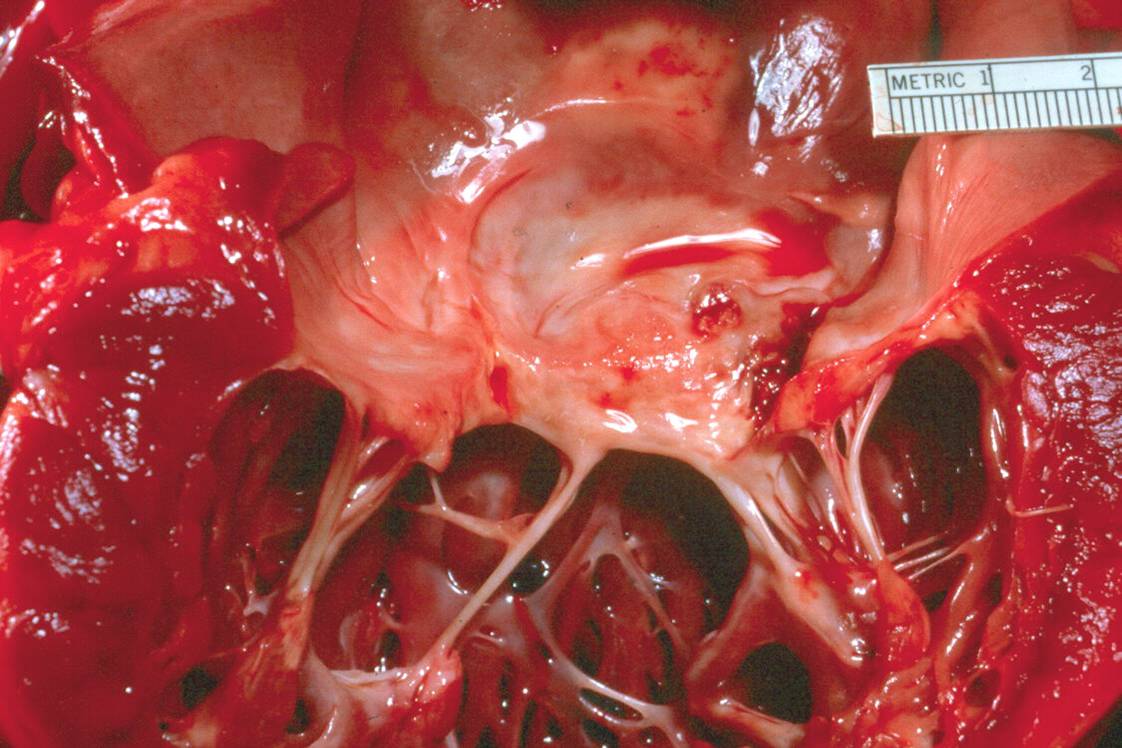
The above
photo is of a mitral valve. The pathology illustrated has developed over a
period of: (1 point
each)
A) 5-6 days
B) 5-6 months
C) at least several years
D) the entire lifetime of a 70 year old
person.
The
initial event starting this disease process was most likely:
A) an episode of diphtheritic myocarditis
B) pharyngitis due to group A
beta–hemolytic streptococci
C) endocarditis due to Streptococcus viridans
During
the acute phase of this disease histopathology is least likely to show:
A) pancarditis
B) bacterial colonies in endocardial
vegetations
C) Aschoff bodies
D) Anitchkow cells
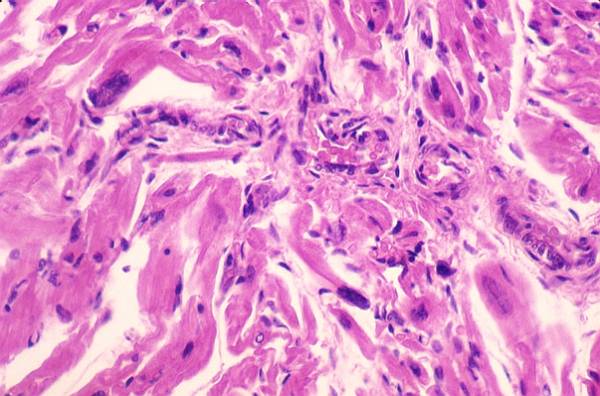
The
following question is related to the photo above. In the photo the large dark
nuclei are indicative of :
(3 points)
A) A rhabdomyoma
B) Glycogen storage disease
C) Myocyte hypertrophy
D) Premalignant dysplasia
E) Mutation of a myosin gene in a case of dilated cardiomyopathy
Fill in
the blanks – 1 word each
(1 point each)
There is
an easily fragmented, “benign” tumor which grows from the endocardium to form a sessile or polypoid mass, usually in the left atrium. It is the most
common primary cardiac tumor in the adult. The name of the tumor is
__MYXOMA___________.
__FIBRINOUS______ pericarditis often develops a few days after onset of
transmural myocardial infarction and occasionally
develops later as Dressler syndrome. (Supply the adjective)
In one or
two sentences describe a clinical scenario which results in cardiac
tamponade. (2 points)
________________________________________________________________________________________________________________________________________________________________________________________________________________________________________________________________________________________________










