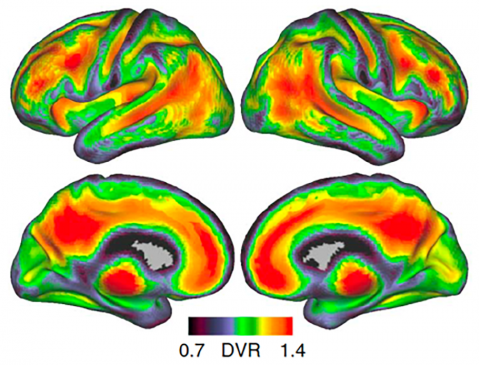
An accumulation of beta-amyloid (Aβ) peptides in the brain is one of the pathological hallmarks of Alzheimer’s disease and presents a high risk of developing the disease. Recent advances in in vivo positron emission tomography (PET) have significantly increased our awareness of the presence of Aβ plaques in approximately 20-50% of asymptomatic older adults who are now considered as preclinical Alzheimer’s disease. Differentiating healthy older adults from those who are in the preclinical stage of Alzheimer’s disease remains challenging, in part because we lack sensitive and specific behavioral and neural measures that detect the presence of Aβ plaques in the preclinical Alzheimer’s disease stage. Furthermore, the co-presence of tau-protein neurofibrillary tangles (NFT), another key pathological marker of Alzheimer’s disease, makes it difficult to link Alzheimer’s pathologies to specific cognitive and brain network dysfunction.
Professor Hwamee Oh and her team study how normal brain aging and Alzheimer’s disease pathology affect cognition and the underlying neural systems in clinically intact older adults with and without Alzheimer’s pathologies. Under the support of an award from the National Institutes of Health, Oh’s group is studying 50 healthy young adults and 125 clinically intact older adults using multimodal neuroimaging approaches that include the-state-of-the-field PET scans that image brain amyloid and tau pathologies and structural and functional MRI. In combination with novel cognitive assessments and neural network analyses of the neuroimaging measurements, Oh’s group hopes to identify more sophisticated behavioral phenotypes and neural markers at the early stage of Alzheimer’s disease pathologies. These findings will enable a non-invasive and more affordable and accessible screening test of the disease with clinical utility in aiding early diagnosis and treatment monitoring.